Advanced Technologies
Orthopaedic surgery lends itself to advanced technologies. These have become increasingly used in recent years, as it has become clear that implant positioning is critical not just to survivorship, but also to function of the prosthetic joint. With improvements in bearing surfaces and materials, joints are less likely to ‘wear out’ and revisions are performed for other reasons.
Dr Young uses these in appropriate settings to optimise implant position and patient function.
Computer Assisted Navigation or “Navigated” surgery
This involves attaching infra-red reflective markers to the bone at the beginning of the case. A computer with an infra red detector is in the operating suite. The surgeon then uses these reflectors and ‘pointer’ to allow the computer to build a model of the joint in space.
Once this is done, the surgeon positions cutting guides with infra-red reflectors. This allows the surgeon to make cuts with one degree or one millimetre accuracy. It also means the surgeon does not have to place instruments in the medullary canal, preventing embolism of bone marrow and fat.
The down side to navigation is the need to have access to computers in theatre as well as potential for fracture through the holes drilled in the bone for reflective markers. Further, the information generated is only as good as the data the surgeon provides, meaning care must still be taken to expose the knee properly and correctly identify landmarks.
Patient Specific Instrumentation
This technology uses imaging (typically an MRI and X rays) to generate a computer model of the knee. The modelling software uses algorithms and 3D measurements to decide where the implants should be positioned to optimise alignment and function. A 3D printer then creates custom cutting guides. These are tailor-made for the individual and are sterilised before being taken to the operating theatre. These then assist the surgeon to make bony cuts.
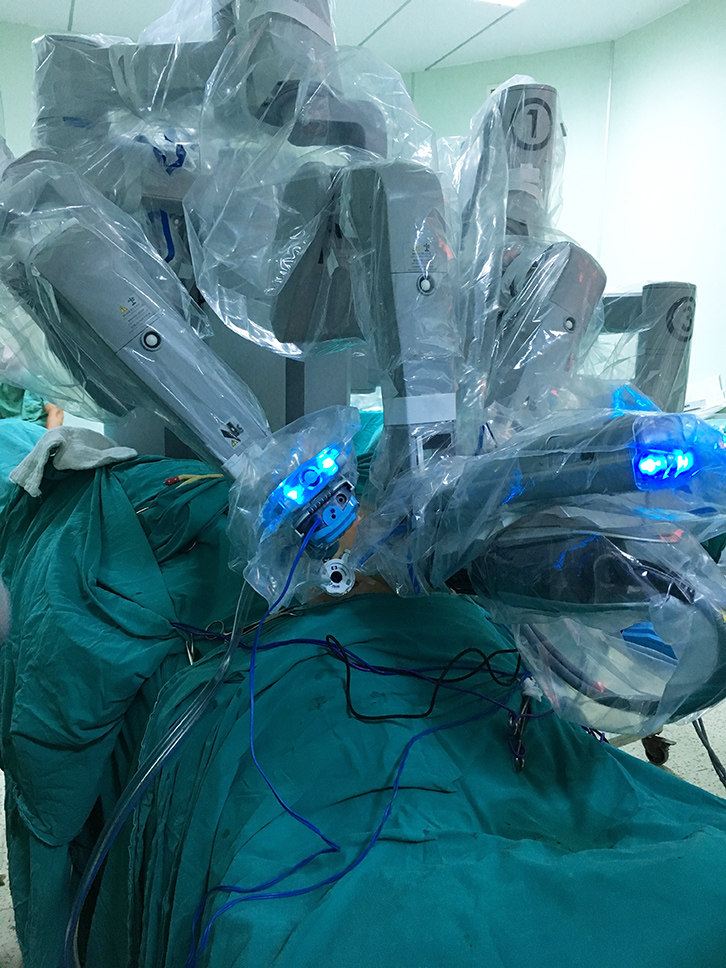
Robotic Surgery
Early robotic surgical devices were fully automated, however they required extensive soft tissue dissection to protect soft tissues and accuracy could be problematic.
Modern orthopaedic surgical robots are now termed passive, as Robotic Surgery is always under manual control by your surgeon at all times, and surgery cannot be automated. Similar to a mix of patient specific instrumentation & navigation based surgery, the surgeon uses various technologies both pre & intra operatively to allow the computer to build a model of the knee and its function.
The surgeon then uses these measurements to decide on component size and position and the computer gives real time feedback on the effect of this on joint function. Once the surgeon is happy with the plan, the robot is brought into play. The robotic arm is loaded with a surgical tool which can only be activated by the surgeon. The computer fixes the position of the robot and only allows the motor to fire if the instruments are cutting according to the planned resection.